Search
- Page Path
- HOME > Search
Original Articles
- Diabetes, Obesity and Metabolism
- EW-7197 Attenuates the Progression of Diabetic Nephropathy in db/db Mice through Suppression of Fibrogenesis and Inflammation
- Kyung Bong Ha, Weerapon Sangartit, Ah Reum Jeong, Eun Soo Lee, Hong Min Kim, Soyeon Shim, Upa Kukongviriyapan, Dae-Kee Kim, Eun Young Lee, Choon Hee Chung
- Endocrinol Metab. 2022;37(1):96-111. Published online February 28, 2022
- DOI: https://doi.org/10.3803/EnM.2021.1305

- 4,027 View
- 182 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Diabetic nephropathy (DN) is characterized by albuminuria and accumulation of extracellular matrix (ECM) in kidney. Transforming growth factor-β (TGF-β) plays a central role in promoting ECM accumulation. We aimed to examine the effects of EW-7197, an inhibitor of TGF-β type 1 receptor kinase (ALK5), in retarding the progression of DN, both in vivo, using a diabetic mouse model (db/db mice), and in vitro, in podocytes and mesangial cells.
Methods
In vivo study: 8-week-old db/db mice were orally administered EW-7197 at a dose of 5 or 20 mg/kg/day for 10 weeks. Metabolic parameters and renal function were monitored. Glomerular histomorphology and renal protein expression were evaluated by histochemical staining and Western blot analyses, respectively. In vitro study: DN was induced by high glucose (30 mM) in podocytes and TGF-β (2 ng/mL) in mesangial cells. Cells were treated with EW-7197 (500 nM) for 24 hours and the mechanism associated with the attenuation of DN was investigated.
Results
Enhanced albuminuria and glomerular morphohistological changes were observed in db/db compared to that of the nondiabetic (db/m) mice. These alterations were associated with the activation of the TGF-β signaling pathway. Treatment with EW-7197 significantly inhibited TGF-β signaling, inflammation, apoptosis, reactive oxygen species, and endoplasmic reticulum stress in diabetic mice and renal cells.
Conclusion
EW-7197 exhibits renoprotective effect in DN. EW-7197 alleviates renal fibrosis and inflammation in diabetes by inhibiting downstream TGF-β signaling, thereby retarding the progression of DN. Our study supports EW-7197 as a therapeutically beneficial compound to treat DN. -
Citations
Citations to this article as recorded by- TGF-β signaling in health, disease, and therapeutics
Ziqin Deng, Tao Fan, Chu Xiao, He Tian, Yujia Zheng, Chunxiang Li, Jie He
Signal Transduction and Targeted Therapy.2024;[Epub] CrossRef - Oxidative stress and inflammation in diabetic nephropathy: role of polyphenols
Qi Jin, Tongtong Liu, Yuan Qiao, Donghai Liu, Liping Yang, Huimin Mao, Fang Ma, Yuyang Wang, Liang Peng, Yongli Zhan
Frontiers in Immunology.2023;[Epub] CrossRef - Beneficial Effects of a Curcumin Derivative and Transforming Growth Factor-β Receptor I Inhibitor Combination on Nonalcoholic Steatohepatitis
Kyung Bong Ha, Eun Soo Lee, Na Won Park, Su Ho Jo, Soyeon Shim, Dae-Kee Kim, Chan Mug Ahn, Choon Hee Chung
Diabetes & Metabolism Journal.2023; 47(4): 500. CrossRef
- TGF-β signaling in health, disease, and therapeutics

- Diabetes, Obesity and Metabolism
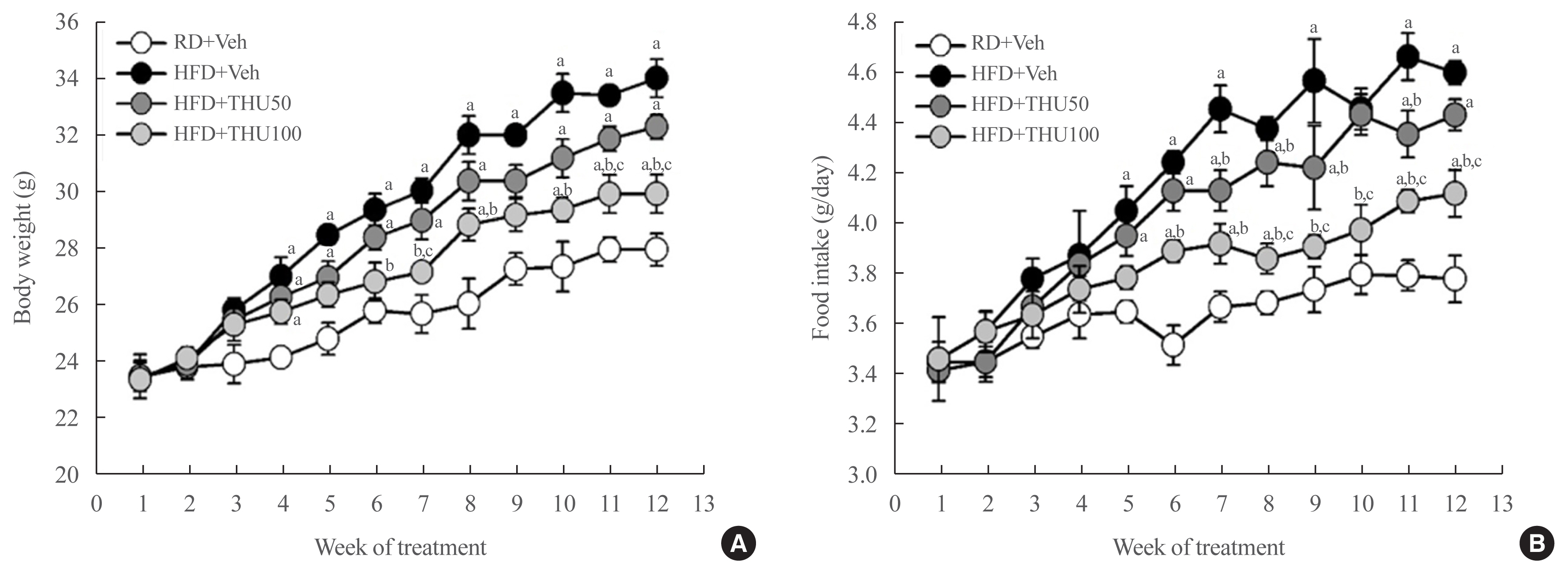
- Tetrahydrocurcumin Ameliorates Kidney Injury and High Systolic Blood Pressure in High-Fat Diet-Induced Type 2 Diabetic Mice
- Weerapon Sangartit, Kyung Bong Ha, Eun Soo Lee, Hong Min Kim, Upa Kukongviriyapan, Eun Young Lee, Choon Hee Chung
- Endocrinol Metab. 2021;36(4):810-822. Published online August 27, 2021
- DOI: https://doi.org/10.3803/EnM.2021.988
- 4,101 View
- 165 Download
- 7 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Activation of the intrarenal renin-angiotensin system (RAS) is implicated in the pathogenesis of kidney injury and hypertension. We aimed to investigate the protective effect of tetrahydrocurcumin (THU) on intrarenal RAS expression, kidney injury, and systolic blood pressure (SBP) in high-fat diet (HFD)-induced type 2 diabetic mice.
Methods
Eight-week-old male mice were fed a regular diet (RD) or HFD for 12 weeks, and THU (50 or 100 mg/kg/day) was intragastrically administered with HFD. Physiological and metabolic changes were monitored and the expression of RAS components and markers of kidney injury were assessed.
Results
HFD-fed mice exhibited hyperglycemia, insulin resistance, and dyslipidemia compared to those in the RD group (P<0.05). Kidney injury in these mice was indicated by an increase in the ratio of albumin to creatinine, glomerular hypertrophy, and the effacement of podocyte foot processes. Expression of intrarenal angiotensin-converting enzyme, angiotensin II type I receptor, nicotinamide adenine dinucleotide phosphate (NADPH) oxidase-4, and monocyte chemoattractant protein-1 was also markedly increased in HFD-fed mice. HFD-fed mice exhibited elevated SBP that was accompanied by an increase in the wall thickness and vascular cross-sectional area (P<0.05), 12 weeks post-HFD consumption. Treatment with THU (100 mg/kg/day) suppressed intrarenal RAS activation, improved insulin sensitivity, and reduced SBP, thus, attenuating kidney injury in these mice.
Conclusion
THU alleviated kidney injury in mice with HFD-induced type 2 diabetes, possibly by blunting the activation of the intrarenal RAS/nicotinamide adenine dinucleotide phosphate oxidase IV (NOX4)/monocyte chemoattractant protein 1 (MCP-1) axis and by lowering the high SBP. -
Citations
Citations to this article as recorded by- The Development of Dyslipidemia in Chronic Kidney Disease and Associated Cardiovascular Damage, and the Protective Effects of Curcuminoids
Zeltzin Alejandra Ceja-Galicia, Ana Karina Aranda-Rivera, Isabel Amador-Martínez, Omar Emiliano Aparicio-Trejo, Edilia Tapia, Joyce Trujillo, Victoria Ramírez, José Pedraza-Chaverri
Foods.2023; 12(5): 921. CrossRef - Translation Animal Models of Diabetic Kidney Disease: Biochemical and Histological Phenotypes, Advantages and Limitations
Wenting Luo, Shiyun Tang, Xiang Xiao, Simin Luo, Zixuan Yang, Wei Huang, Songqi Tang
Diabetes, Metabolic Syndrome and Obesity.2023; Volume 16: 1297. CrossRef - Curcumin ameliorates focal segmental glomerulosclerosis by inhibiting apoptosis and oxidative stress in podocytes
Hui Zhang, Qing-Qing Dong, Hua-Pan Shu, Yu-Chi Tu, Qian-Qian Liao, Li-Jun Yao
Archives of Biochemistry and Biophysics.2023; 746: 109728. CrossRef - An examination of the protective effects and molecular mechanisms of curcumin, a polyphenol curcuminoid in diabetic nephropathy
Xiaoyu Zhu, Xingli Xu, Chigang Du, Yanping Su, Lixue Yin, Xiaoqiu Tan, Hui Liu, Yiru Wang, Lei Xu, Xinghua Xu
Biomedicine & Pharmacotherapy.2022; 153: 113438. CrossRef - An integrated bioinformatics analysis and experimental study identified key biomarkers CD300A or CXCL1, pathways and immune infiltration in diabetic nephropathy mice
WEI LIANG, QIANG LUO, ZONGWEI ZHANG, KEJU YANG, ANKANG YANG, QINGJIA CHI, HUAN HU
BIOCELL.2022; 46(8): 1989. CrossRef
- The Development of Dyslipidemia in Chronic Kidney Disease and Associated Cardiovascular Damage, and the Protective Effects of Curcuminoids

Case Reports
- 1-34 PTH Could Reverse Impaired Bone Mineralization Induced By the Overdose of Bisphosphonate.
- Kyeong Hye Park, Kwang Joon Kim, Han Seok Choi, Kyoung Min Kim, Eun Young Lee, Seonhui Han, Hyun Sil Kim, Daham Kim, Hannah Seok, Eun Yeong Choe, Yumie Rhee, Sung Kil Lim
- Endocrinol Metab. 2012;27(3):247-250. Published online September 19, 2012
- DOI: https://doi.org/10.3803/EnM.2012.27.3.247
- 12,690 View
- 27 Download
-
 Abstract
Abstract
 PDF
PDF - Bisphosphonates are the mainstay of osteoporosis treatment. Despite the fact that bisphosphonates have a relatively good safety record and are tolerated well by the majority of patients, serious adverse events have been associated with their use. A 41-year-old man had been diagnosed with osteoporosis and had taken etidronate 200 mg/day daily for 2 years due to the judgmental error. He was referred for the management of refractory bone pain and generalized muscle ache. Serum calcium, phosphate, 25-hydroxy-vitamin D (25(OH)D), and immunoreactive parathyroid hormone (iPTH) were within normal range. Plain X-ray showed multiple fractures. Whole body bone scan confirmed multiple sites of increased bone uptakes. Tetracycline-labeled bone biopsy showed typical findings of osteomalacia. He was diagnosed with iatrogenic, etidronate-induced osteomalacia. The patient received daily parathyroid hormone (PTH) injection for 18 months. PTH effectively reverses impaired bone mineralization caused by etidronate misuse. Currently, he is doing well without bone pain. Bone mineral density significantly increased, and the increased bone uptake was almost normalized after 18 months. This case seems to suggest that human PTH (1-34) therapy, possibly in association with calcium and vitamin D, is associated with important clinical improvements in patients with impaired bone mineralization due to the side effect of bisphosphonate.

- A Case of Pituitary Adenoma with Simultaneous Secretion of TSH and GH.
- Eun Young Lee, Cheol Ryong Ku, Hyun Min Kim, Woo Kyoung Lee, Jung Soo Lim, Sena Hwang, Do Hwan Kim, Dong Yeob Shin, Eun Jig Lee
- Endocrinol Metab. 2011;26(2):160-165. Published online June 1, 2011
- DOI: https://doi.org/10.3803/EnM.2011.26.2.160
- 2,979 View
- 30 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - Thyrotropin (TSH)-secreting pituitary adenoma is a very rare disease. In one-quarter of patients suffering from this disease, the pituitary tumor secretes other anterior pituitary hormones. Herein, we report a case of pituitary adenoma with simultaneous secretion of TSH and growth hormone (GH). A 34-year-old female visitied local hospital complaining of sweating, intermittent palpitation, and weight loss of 8 kg within 1 year. The patient had undergone trans-sphenoidal surgery 3 years prior for resolution of a TSH and GH co-secreting pituitary adenoma. She had been administered somatostatin analogue prior to visiting our hospital. The patient's GH levels were suppressed to below 1 ng/mL on the 75 g oral glucose tolerance test, and her basal insulin-like growth factor-I (IGF-I) level was within normal range. Thyroid function tests demonstrated increased levels of both free thyroxine and TSH. Sella-MRI revealed pituitary adenoma at the floor of the pituitary fossa, approximately 2 cm in height. Therefore, she was diagnosed with residual TSH-secreting pituitary adenoma. The patient again underwent trans-sphenoidal surgery and entered complete remission, based on hormone levels and MRI findings.
-
Citations
Citations to this article as recorded by- Endoscopic Transsphenoidal Surgery of Pituitary Adenomas: Preliminary Results of the Neurosurgery Service of Hospital Cristo Redentor
Gerson Perondi, Afonso Mariante, Fernando Azambuja, Gabriel Frizon Greggianin, Wanderson William dos Santos Dias, Giulia Pinzetta
Arquivos Brasileiros de Neurocirurgia: Brazilian Neurosurgery.2023; 42(02): e89. CrossRef - A case of a co-secreting TSH and growth hormone pituitary adenoma presenting with a thyroid nodule
Laura Hamilton Adams, Derick Adams
Endocrinology, Diabetes & Metabolism Case Reports.2018;[Epub] CrossRef
- Endoscopic Transsphenoidal Surgery of Pituitary Adenomas: Preliminary Results of the Neurosurgery Service of Hospital Cristo Redentor

- Primary Bilateral Adrenal Non-Hodgkin's Lymphoma Presented with Adrenal Insufficiency: A Case Report.
- Eun Young Lee, Kyoung Min Kim, Kwang Joon Kim, Songmi Noh, Jin Seok Kim, Woo Ik Yang, Sung Kil Lim
- Endocrinol Metab. 2011;26(1):101-105. Published online March 1, 2011
- DOI: https://doi.org/10.3803/EnM.2011.26.1.101
- 1,820 View
- 23 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Primary adrenal lymphoma is a very rare disease and it is known to have a poor prognosis. We report here on a case of primary adrenal insufficiency that was secondary to primary bilateral adrenal lymphoma. A 54-year old man was hospitalized because of easy fatigability, weight loss and consistent malaise for 6 months. The physical examination revealed hyperpigmentation on the anterior chest and hypotension. According these findings and symptoms, we did a rapid ACTH stimulation test with a clinical suspicion of adrenal insufficiency. He showed an inadequate adrenal response and so he was diagnosed with adrenal insufficiency. The abdominal CT images showed bilateral huge adrenal masses and increased uptake of the adrenal glands on PET. The pathologic diagnosis by ultrasound-guided gun biopsy of the right adrenal gland was diffuse large B cell lymphoma. The patient was administered combination chemotherapy with the R-CHOP regimen, and after 8-cycles of chemotherapy, he achieved complete remission of tumor according to the image studies and he recovered his adrenal function. Primary adrenal lymphoma, although a rare disease, should be considered in patients with bilateral enlargement of the adrenal glands and when the adrenal glands show increased uptake on a PET scan, and especially there is adrenal insufficiency.
-
Citations
Citations to this article as recorded by- Systemic vs. intrathecal central nervous system prophylaxis in primary adrenal/renal diffuse large b-cell Lymphoma: A multi-institution retrospective analysis and systematic review
John Xie, Albert Jang, Motohide Uemura, Shigeaki Nakazawa, Teresa Calimeri, Andres JM Ferreri, Shuang R. Chen, Janet L. Schmid, Theresa C. Brown, Francisco Socola, Hana Safah, Nakhle S. Saba
Leukemia Research Reports.2021; 16: 100263. CrossRef
- Systemic vs. intrathecal central nervous system prophylaxis in primary adrenal/renal diffuse large b-cell Lymphoma: A multi-institution retrospective analysis and systematic review

Original Articles
- Correlation between Pituitary Insufficiency and Magnetic Resonance Imaging Finding in Non-Functioning Pituitary Adenomas.
- Hyun Min Kim, Cheol Ryong Ku, Eun Young Lee, Woo Kyung Lee, Jung Soo Lim, Sena Hwang, Mi Jung Lee, Seung Ku Lee, Sun Ho Kim, Eun Jig Lee
- Endocrinol Metab. 2010;25(4):310-315. Published online December 1, 2010
- DOI: https://doi.org/10.3803/EnM.2010.25.4.310
- 2,053 View
- 28 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Non-functioning pituitary adenomas (NFPAs) are characterized by the absence of clinical and biochemical evidence of pituitary hormone hypersecretion, and these tumors constitute approximately one third of all the tumors of the anterior pituitary. Recently, hormonal deficiencies have gradually evolved to become the leading presenting signs and symptoms in patients with NFPAs. We investigated pituitary hormonal insufficiencies according to the magnetic resonance imaging (MRI) findings in patients with NFPA. METHODS: We evaluated the patients who were newly diagnosed with NFPA from 1997 through 2009. Among them, we analyzed 387 patients who were tested for their combined pituitary function and who underwent MRI. The severity of the hypopituitarism was determined by the number of deficient axes of the pituitary hormones. On the MRI study, the maximal diameter of the tumor, Hardy's classification, the thickness of the pituitary gland and the presence of stalk compression were evaluated. RESULTS: The mean age was 46.85 +/- 12.93 years (range: 15-86) and 186 patients (48.1%) were male. As assessed on MRI, the tumor diameter was 27.87 +/- 9.93 mm, the thickness of the normal pituitary gland was 1.42 +/- 2.07 mm and stalk compression was observed in 201 patients (51.9%). Hypopituitarism was observed in 333 patients (86.0%). Deficiency for each pituitary hormone was most severe in the patients with Hardy type IIIA. Hypopituitarism was severe in the older age patients (P = 0.001) and the patients with a bigger tumor size (P < 0.001) and the presence of stalk compression (P < 0.001). However, the patients who had a thicker pituitary gland showed less severe hypopituitarism (P < 0.001). Multivariate analysis showed that age, tumor diameter and the thickness of pituitary gland were important determinants for pituitary deficiency (P = 0.004, P < 0.001, P = 0.022, respectively). CONCLUSION: The results suggest that the hormonal deficiencies in patient with NFPA were correlated with the MRI findings, and especially the tumor diameter and preservation of the pituitary gland. -
Citations
Citations to this article as recorded by- Clinical Parameters to Distinguish Silent Corticotroph Adenomas from Other Nonfunctioning Pituitary Adenomas
Daham Kim, Cheol Ryong Ku, Se Hee Park, Ju Hyung Moon, Eui Hyun Kim, Sun Ho Kim, Eun Jig Lee
World Neurosurgery.2018; 115: e464. CrossRef
- Clinical Parameters to Distinguish Silent Corticotroph Adenomas from Other Nonfunctioning Pituitary Adenomas

- p53, p21 and bcl-2 Protein Expressions and the Clinical Significance in Papillary Thyroid Carcinoma.
- Tae Sik Jung, Keun Sook Kim, Young Lyun Oh, Jung Hwa Jung, Eun Young Lee, Hye Seung Jung, Yong Ki Min, Myung Shik Lee, Moon Kyu Lee, Kwang Won Kim, Jae Hoon Chung
- J Korean Endocr Soc. 2007;22(2):98-104. Published online April 1, 2007
- DOI: https://doi.org/10.3803/jkes.2007.22.2.98
- 1,847 View
- 18 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
There have been some investigations concerning the role of p53, p21 and bcl-2 protein expressions for the tumorigenesis of thyroid cancer. It had been debated that these protein expressions were associated with aggressive features of papillary thyroid carcinoma. We studied to evaluate the prevalence of these protein expressions and their clinical significances in papillary thyroid carcinoma. METHODS: We selected 49 patients with papillary thyroid carcinoma who had been operated on at Samsung Medical Center during the last 10 years. Immunohistochemical staining for p53, p21 and bcl-2 was done by the use of paraffin embedded tissues. We analyzed the results of immunohistochemical staining for p53, p21 and bcl-2 and the correlation with the patients' age, gender, tumor size, multifocality, tumor invasion to both lobes, extrathyroidal invasion, cervical lymph node invasion, distant metastasis and the clinical outcomes. RESULTS: Immunohistochemical staining for p53 was positive in 10 patients (20%), p21 was positive in 36 patients (73%) and bcl-2 was positive in 18 patients (37%). The p53 and bcl-2 expressions were not associated with the clinical parameters. Tumor multifocality and extrathyroidal invasion were significantly higher in the p21 positive group (both P < 0.05). CONCLUSION: This study showed that the p21 protein expression was associated with tumor multifocality and extrathyroidal invasion in the patients with papillary thyroid carcinoma. Immunohistochemical stains for p21 may be used as a parameter for tumor aggressiveness in papillary thyroid carcinoma. -
Citations
Citations to this article as recorded by- Clinicopathologic and Diagnostic Significance of p53 Protein Expression in Papillary Thyroid Carcinoma
Mi Kyung Shin, Jeong Won Kim
Asian Pacific Journal of Cancer Prevention.2014; 15(5): 2341. CrossRef
- Clinicopathologic and Diagnostic Significance of p53 Protein Expression in Papillary Thyroid Carcinoma

Case Reports
- A case of Methimazole-Induced Cholestatic Jaundice With Agranulocytosis.
- Sang Gu Kang, Jong Oh Bae, Eun Young Lee, Seong Min Lim, Sang Kun Cho, Ji Hye Kim, Sun Kyung Song
- J Korean Endocr Soc. 2005;20(5):519-523. Published online October 1, 2005
- DOI: https://doi.org/10.3803/jkes.2005.20.5.519
- 2,087 View
- 25 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - Methimazole is a widely used and generally well-tolerated antithyroid agent. Adverse reactions occur in 1~5% of patients taking methimazole medication, but these are most commonly transient, benign leukopenia and a skin rash. Severe cholestatic jaundice, combined with agranulocytosis, has been known as a rare complication. Herein, a case of methimazole induced cholestatic jaundice, with agranulocytosis, is reported.
-
Citations
Citations to this article as recorded by- A Case Report of Methimazole-Induced Acute Liver Failure Successfully Treated with Liver Transplantation
Sung Jin Jeon, Tae Yong Kim, Seung-Hoon Lee, Jong Sik Kang, Gwang Hyeon Choi, Seung-Gyu Lee, Hee Sang Hwang
Korean Journal of Medicine.2012; 83(3): 363. CrossRef - A Case of Methimazole-induced Pancytopenia: Successful Treatment with Recombinant Human Granulocyte Colony-stimulating Factor
Joo Hyoung Lee, Jihyun Lee, Sang Hun Sung, Sung Hwa Bae, Sang Gyung Kim, Hoon Kyu Oh
Journal of Korean Endocrine Society.2006; 21(6): 548. CrossRef
- A Case Report of Methimazole-Induced Acute Liver Failure Successfully Treated with Liver Transplantation

- Upper Airway Obstruction Caused by Intratracheal Ectopic Thyroid Tissue during Pregnancy.
- Eun Young Lee, Byung Wan Lee, Jhingook Kim, Sung Jin Bae, Tae Sik Jung, Hye Seung Jung, Yong Ki Min, Myung Shik Lee, Moon Kyu Lee, Kwang Won Kim, Jae Hoon Chung
- J Korean Endocr Soc. 2005;20(4):413-420. Published online August 1, 2005
- DOI: https://doi.org/10.3803/jkes.2005.20.4.413
- 1,861 View
- 18 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Herein is report an extremely rare case of an intratracheal ectopic thyroid gland related with pregnancy. A 34-year-old woman, in gestational week 11, presented with stridor, progressive dyspnea and a choking sensation during her second pregnancy. Computed tomography of the neck and chest revealed a round intratracheal mass obstructing the airway. A bronchoscopic biopsy with LASER cauterization was performed, and the histological finding revealed normal thyroid tissue. The external thyroid of the patient was evaluated, but only found benign nodules in the thyroid gland. She underwent a segmental resection of the trachea, including the mass and the 1st tracheal cartilage. The histological findings revealed the intratracheal mass to be composed of benign thyroid tissue with nodular hyperplasia. After surgery, no pulmonary symptoms were evident. This case suggested the effect of pregnancy on thyroid tissue stimulatied due to a combination of an increasing human chorionic gonadotropin(hCG) level and relative iodine deficiency during pregnancy. This is the first report on the detection of intratracheal ectopic thyroid tissue during pregnancy in Korea.
-
Citations
Citations to this article as recorded by- A case of mediastinal ectopic thyroid presenting with a paratracheal mass
Eun Roh, Eun Shil Hong, Hwa Young Ahn, So-Yeon Park, Ho Il Yoon, Kyong Soo Park, Young Joo Park
The Korean Journal of Internal Medicine.2013; 28(3): 361. CrossRef
- A case of mediastinal ectopic thyroid presenting with a paratracheal mass


 KES
KES

 First
First Prev
Prev



